Optimizing metabolic health is very important for longevity. This month, we discuss the importance of maintaining optimal blood sugar levels to avoid insulin resistance and its more severe manifestation, type 2 diabetes.
The Ins and Outs of Diabetes
It is estimated that more than 37 million people in the United States have Diabetes. Among U.S. adults ages 18 years or older, 96 million (over one-third) have prediabetes, and more than 8 out of 10 of them don’t know they have it.
Diabetes is the eighth leading cause of death in the United States according to the CDC. It is also a major contributor to the top three leading causes of death which are cardiovascular disease, Cancer and Alzheimer’s related dementia.
Diabetes is a result of problems with the pancreatic hormone insulin. Insulin controls the amount of blood sugar (glucose) circulating in the blood and the rate at which it is absorbed into cells in our body. Glucose is the body’s primary fuel. Brain, muscle, and liver tissues are types of cells that rely on glucose in order to perform optimally. Having too much or too little glucose in the bloodstream is disruptive to your metabolism.
Poor blood sugar regulation is the precursor to insulin resistance. Insulin resistance is defined as an inability of insulin to facilitate glucose uptake from the blood into the cells. This makes it difficult for key tissues such as the brain, muscles, and liver to effectively use glucose as fuel.
Insulin resistance is a leading risk factor in the development of type 2 diabetes, cardiovascular disease, cancer, cognitive decline/Alzheimer’s, kidney disease, obesity, blindness, nerve disorders, polycystic ovary disease (PCOS), non-alcoholic fatty liver disease (NAFLD), NASH, and inflammation.
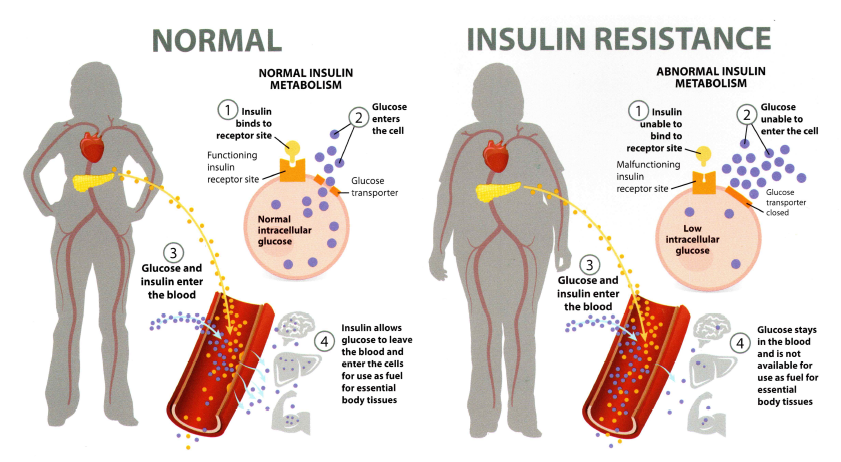
The food you eat is broken down into blood sugar. This enters our bloodstream signaling our pancreas to release insulin. Insulin transports blood sugar into our cells for energy. It also triggers the liver to store blood sugar for later use. Glucose enters our cells, levels in our blood decrease which signals insulin levels to decrease.
What Happens in Type 2 Diabetes
Insulin secretion is normal or high normal but it is not recognized by the body’s cells in people with type 2 diabetes. The pancreas works harder producing more insulin to push blood glucose into the cells. Excess blood glucose is inflammatory to our body and needs to be moved into cells as soon as possible.
Insulin levels rise telling the liver and muscle tissues to store blood sugar. When these tissues are full, the liver sends excess blood sugar to adipose tissue where it is stored in fat cells. This leads to weight gain primarily in the abdominal area and is called “visceral fat”.
Now, subcutaneous fat is thought to be rather harmless — this visceral fat is anything but harmless. These fat cells promote immune cell activation and secrete inflammatory cytokines such as TNF-alpha and IL-6, key markers and drivers of inflammation, in the midst of your most important bodily organs. This may be why visceral fat is linked to an increased risk of both cancer and cardiovascular disease.
Getting Tested and Addressing Diabetes
A fasting blood sugar test measures your blood sugar after an overnight fast (not eating for 8 hours). According to the CDC, a fasting blood sugar level of 99 mg/dL or lower is normal, 100 to 125 mg/dL indicates prediabetes, and 126 mg/dL or higher indicates you have diabetes.

The end goal in type 2 diabetes is to lower blood glucose. The goal should be to increase insulin sensitivity at the tissue level which will result in a reduction in blood glucose.
Addressing high blood sugar/insulin resistance should always start with lifestyle changes.
Dietary modifications such as eating more whole, unprocessed foods, limiting refined carbohydrates and simple sugars, increasing intake of organic vegetables, fruits and whole grains, lean protein, and increasing dietary fiber are a great starting point.
The Mediterranean diet is a good dietary plan to follow. Eat your final meal of the day no later than 6 PM. This allows your food to digest before you go to bed. Time restricted eating (also referred to as intermittent fasting) is very helpful for some people.
Increasing regular exercise and physical activity is one of the best ways to improve your body’s insulin sensitivity. This helps move blood glucose into the muscle tissue where it is used as energy. Try to get 150 minutes each week of moderate physical activity. An exercise routine that includes a combination of aerobic exercise and strength training seems most effective in lowering blood sugar and improving insulin sensitivity.
Getting good sleep (8 to 9 hours each night) and reducing stress levels (see our Managing Chronic Stress blog) are also important for managing blood sugar. Studies have shown that sleep deprivation, 4 hours per night or less, raises blood sugar and makes the body more insulin resistant. Deep breathing and meditation may help improve sleep and manage stress.
Supplements, vitamins, and key phyto-nutrients have known roles in supporting blood sugar balance and regulation in the body. Supplements we recommend include Alpha lipoic acid, Berberine, Essential fatty acids found in Omega-3 fish oil, Magnesium, B-vitamins, chromium, and Vanadium. There are also herbal extracts that support normal blood sugar levels such as cinnamon, bitter melon, Gymnema, Fenugreek, and Bergamot. These nutrients can be found in the products CM Core and Diaxinol. We also carry Medical Foods like Ultra Glucose Control and UltraMeal Cardio 360, formulated to support the nutritional management of glucose response.
Please contact our pharmacy for more information.
May Monthly specials 15% off the following products: CM Core, Diaxinol, Reacted Magnesium, OrthoMega fish oil, Orthobiotic, ProOmega Blood Sugar, Berberine VasQx, Ultra Glucose Control, and Freestyle Libre 3 CGM.

Reacted Magnesium
Dietary Supplement
Berberine VasoQX
Cardiovascular and Glycemic Support Dietary Supplement

OrthoMega Fish Oil
Dietary Supplement

Ortho Biotic
Dietary Supplement

Pro Omega Blood Sugar
Dietary Supplement

Ultra Glucose Control
Support for the Nutritional Management of Glucose Response
Here to help.
Contact Morgan Compounding Pharmacy today with questions on how we can help you with recommendations to manage your blood sugar and insulin resistance.